October 18, 2010
Why Zyprexa (And Other Atypical Antipsychotics) Make You Fat

this post does not apply to her, she only eats apples
Strange finding: Zyprexa makes free fatty acids level go down.
Wait, isn't that a good thing?
II. Zyprexa's effects on glucose and insulin are bad.
In a rat study of rats, using rats, Zyprexa raised glucose levels by 20%, both in fed and fasting states.
It didn't much increase insulin in fed states (already high) but it kept insulin high even in fasting states: at 14h post meal, it was 140% higher than it should have been. All that exposure to insulin, for so long. At the coffee cart, we doctors would call that bad.
III. Zyprexa's effect on triglycerides is... weird.
Zyprexa made circulating triglyceride levels fall-- it promoted the uptake of free fatty acids by various tissues:
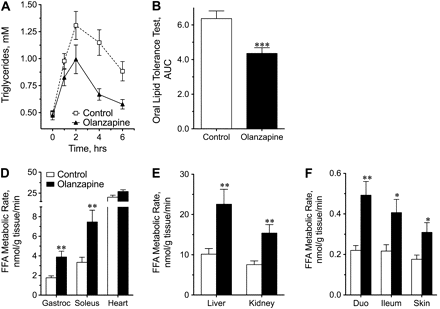
All those tissues taking up fatty acids-- what did they do with it?
IV. Zyprexa Makes Your Body Use Fat, Not Carbs, As Fuel
Normally, after eating, your body uses carbohydrate as the main energy source. After a long time hungry, it switches to fat.
Zyprexa made the body use fat all the time:
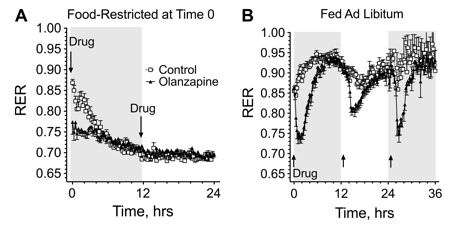
RER (respiratory exchange ratio) tells you what's being used: 1= carbs, 0.85= carb/fat mix, and .7 is all fat. You eat, and your body uses carbs. After a few hours, your body switches to fat utilization.
In graph A, in the first 3 hours the body should have been using carbs and fat; but with Zyprexa, it was preferring mostly fat.
In graph B, every time you got a Zyprexa dose, your body switched to fat utilization instead of carbs.
V. Wait a second, why would increased utilization of fat be a bad thing?
If the body is churning through the fat, what do you think it is doing with all the sugar? Answer: turning your arteries into Twizzlers. Yum!
The typical thinking is that hyperglycemia leads to insulin resistance leads to increased fatty acid utilization. But that might be the wrong direction: it seems that the increased fatty acid utilization means sugar is unused (hyperglycemia) and remains high well into the fasting state, with consequent high levels of insulin. Insulin high too long becomes tolerance to insulin becomes insulin resistance becomes BKA.
VI. SUMMARY: A class effect, to varying degrees; and eating less may not help.
1. Food intake was the same between controls and Zyprexaers. You get these effects even if you eat the same.
2. This effect is shared by other atypicals, in a predictable fashion:
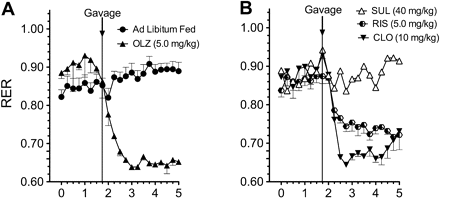 In the fed state, Zyprexa and Clozaril do a massive conversion to fat utilization, Risperdal a medium, and sulpiride minimal covnersion.
In the fed state, Zyprexa and Clozaril do a massive conversion to fat utilization, Risperdal a medium, and sulpiride minimal covnersion.
In the fasting state:
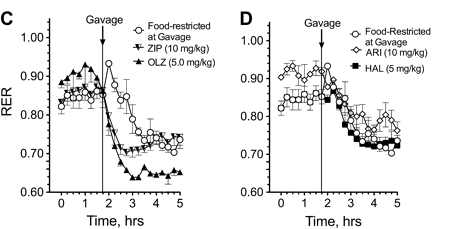 Geodon has a lesser effect than Zyprexa, and appears to normalize; Abilify and Haldol seem close to normal.
Geodon has a lesser effect than Zyprexa, and appears to normalize; Abilify and Haldol seem close to normal.
3. These effects are consistent with Lilly's own studies that the majority of weight gain happens in the first month, and not suddenly after a year of use.
4. There is still a hunger component to weight gain that is separate from the metabolic effect. Some drugs will make you hungry, change your metabolism, or some mixture of the two. Hunger appears to be a H1 mediated process (Seroquel, Zyprexa, Clozaril, Remeron, Paxil>Prozac, etc.)
5. The immediate clinical consequence of this information is probably (paradoxically) to tell the patients to eat less sugar.
Unless you dramatically cut fat out of your diet, the body will still churn through what fat you do eat at the expense of carbohydrate. Better, and easier, to reduce the carb load that lingers in your body (and likely ultimately gets stored.)
VII. Is that all the bad news?
No, of course not!
In another study (same authors, same topic, same time-- two completely different journals; thanks promotions committee, turning academics into bloggers one study at a time) they found that while there was increased lipogenesis (storage), the rats didn't have a change in body weight.
In other words, Zyprexa didn't make them heavier, it made them fatter. It increased their body fat while decreasing the lean body mass. Bright side: now they can float!
Add to this that it though caloric intake was the same, it dramatically decreased locomotor activity. So same calories, but less calorie need.
VIII. Well thank God doctors are finally going to know the truth about Zyprexa!
From who(m)?
The reality is I found these two articles by accident, researching a blog post about something else entirely. I would never have found this article, let alone the other article, on my own. And I read a lot.
Ordinarily, this kind of information would have come to me through my Abilify rep: "see? Zyprexa blows!" But the FDA now forbids anti-competitor comparisons; and neither are the reps allowed to tell me that the study exists. Promotional speakers can't mention this either. So? CME? BWAHAHAHAHAHAHAHAHA!
Here's the bottom line, and it applies to all speech everywhere: either you permit all kinds of speech, and let the truth battle on its merits; or you permit only one line of speech-- and let the truth, if it was suppressed, come up like smoke through cracks. But when you permit some speech and block others-- when you create gatekeepers of speech-- it creates the impression that the truth is in the permitted speech. Most of the time, it's not.
IV. Zyprexa Makes Your Body Use Fat, Not Carbs, As Fuel
Normally, after eating, your body uses carbohydrate as the main energy source. After a long time hungry, it switches to fat.
Zyprexa made the body use fat all the time:

RER (respiratory exchange ratio) tells you what's being used: 1= carbs, 0.85= carb/fat mix, and .7 is all fat. You eat, and your body uses carbs. After a few hours, your body switches to fat utilization.
In graph A, in the first 3 hours the body should have been using carbs and fat; but with Zyprexa, it was preferring mostly fat.
In graph B, every time you got a Zyprexa dose, your body switched to fat utilization instead of carbs.
V. Wait a second, why would increased utilization of fat be a bad thing?
If the body is churning through the fat, what do you think it is doing with all the sugar? Answer: turning your arteries into Twizzlers. Yum!
The typical thinking is that hyperglycemia leads to insulin resistance leads to increased fatty acid utilization. But that might be the wrong direction: it seems that the increased fatty acid utilization means sugar is unused (hyperglycemia) and remains high well into the fasting state, with consequent high levels of insulin. Insulin high too long becomes tolerance to insulin becomes insulin resistance becomes BKA.
VI. SUMMARY: A class effect, to varying degrees; and eating less may not help.
1. Food intake was the same between controls and Zyprexaers. You get these effects even if you eat the same.
2. This effect is shared by other atypicals, in a predictable fashion:
 In the fed state, Zyprexa and Clozaril do a massive conversion to fat utilization, Risperdal a medium, and sulpiride minimal covnersion.
In the fed state, Zyprexa and Clozaril do a massive conversion to fat utilization, Risperdal a medium, and sulpiride minimal covnersion.In the fasting state:
 Geodon has a lesser effect than Zyprexa, and appears to normalize; Abilify and Haldol seem close to normal.
Geodon has a lesser effect than Zyprexa, and appears to normalize; Abilify and Haldol seem close to normal.3. These effects are consistent with Lilly's own studies that the majority of weight gain happens in the first month, and not suddenly after a year of use.
4. There is still a hunger component to weight gain that is separate from the metabolic effect. Some drugs will make you hungry, change your metabolism, or some mixture of the two. Hunger appears to be a H1 mediated process (Seroquel, Zyprexa, Clozaril, Remeron, Paxil>Prozac, etc.)
5. The immediate clinical consequence of this information is probably (paradoxically) to tell the patients to eat less sugar.
Unless you dramatically cut fat out of your diet, the body will still churn through what fat you do eat at the expense of carbohydrate. Better, and easier, to reduce the carb load that lingers in your body (and likely ultimately gets stored.)
VII. Is that all the bad news?
No, of course not!
In another study (same authors, same topic, same time-- two completely different journals; thanks promotions committee, turning academics into bloggers one study at a time) they found that while there was increased lipogenesis (storage), the rats didn't have a change in body weight.
In other words, Zyprexa didn't make them heavier, it made them fatter. It increased their body fat while decreasing the lean body mass. Bright side: now they can float!
Add to this that it though caloric intake was the same, it dramatically decreased locomotor activity. So same calories, but less calorie need.
VIII. Well thank God doctors are finally going to know the truth about Zyprexa!
From who(m)?
The reality is I found these two articles by accident, researching a blog post about something else entirely. I would never have found this article, let alone the other article, on my own. And I read a lot.
Ordinarily, this kind of information would have come to me through my Abilify rep: "see? Zyprexa blows!" But the FDA now forbids anti-competitor comparisons; and neither are the reps allowed to tell me that the study exists. Promotional speakers can't mention this either. So? CME? BWAHAHAHAHAHAHAHAHA!
Here's the bottom line, and it applies to all speech everywhere: either you permit all kinds of speech, and let the truth battle on its merits; or you permit only one line of speech-- and let the truth, if it was suppressed, come up like smoke through cracks. But when you permit some speech and block others-- when you create gatekeepers of speech-- it creates the impression that the truth is in the permitted speech. Most of the time, it's not.
POLL: What was the "other research" I was doing?
71 Comments